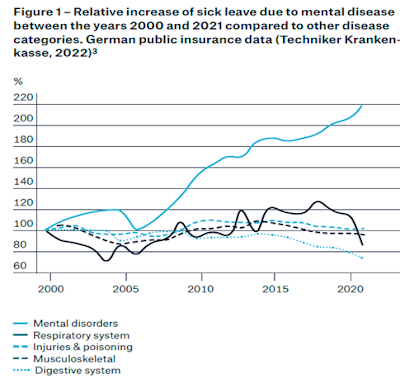
Last time, we outlined the growth in mental disorder/psychological injury claims in workers' compensation and related workplace insurance programs.
Despite data gaps, the trends in many jurisdictions
show an increasing number and proportion of accepted work-related mental injury
and disability claims; there is some evidence that mental disability claims in
the broader social insurance environment may be a more consistent proportion of
disability types.
In this part, we
will explore the underlying changes that may be contributing to the observed
trend, explain why comparison between jurisdictions is challenging at best, and
touch on initiatives for prevention and
treatment.
Attitudes
about mental injuries
In August 1943, General George S. Patton encountered Private Charles Kuhl in the 15th Evacuation Field Hospital at
Nicosia (Sicily). The eighteen-year-old Kuhl had been pulled from battle
suffering from "battle fatigue" as well as malaria and dysentery. Patton asked him
about his injuries. "I guess I can't take it," Kuhl
told the General. Patton grabbed the young soldier by the collar and slapped
him with a leather glove, describing him later in writing as a "weakling". A few
days later at an evacuation hospital in San Stephano, the general encountered
Pvt. Paul Bennet, age 21, having been evacuated from the fighting for
exhaustion and dehydration. Bennet told the general, "It's my nerves, I can't take
the shelling anymore". The general struck Bennet
and called him a coward.
The incidents of Patton slapping or deriding soldiers
as cowards were covered extensively in the newspaper headlines of the day.
Public and political leadership recognized that the
General had gone too far. Not far enough for Eisenhower to
order Patton's removal from command but
enough to get Patton to apologize.
Our collective understanding of mental injuries has
evolved, but there are persistent
undercurrents of belief that any mental disability is the fault of the
individual, an inherent weakness. "Toughen
up!" is still the default
response of many, but public acceptance towards the reality of mental injuries
has improved. The Roper Center for Public Opinion Research notes on its Public
Attitudes about Mental Health webpage [ https://ropercenter.cornell.edu/public-attitudes-about-mental-health ] :
Sixty-seven percent of the public believed that mental
disorders were an extreme or serious public health problem.
Eighty-nine percent believed that physical and mental
health were equally significant.
Attitudes have changed and are changing over time. That
change has spurred policymakers to become
more specific in creating avenues for the
treatment of and compensation for mental injuries. That said, attitudes toward
mental illness still vary not only by
jurisdiction but by industry, and even
by occupation or specific worksite. The
toughen-up attitude still exists.
On the disability insurance side, this shift has meant
changes to policies and procedures. While not everyone has access to disability
plans, insured parties want clarity of the coverage; insurers need clear procedures to approve
coverage. Disability insurers also want to limit their liability to non-work-related
cases.
For workers’ compensation, growing recognition of the
work-relatedness of mental injuries requires changes to legislation and policy
allowing for compensation. Workers’ compensation is typically the first payer
for temporary disability so decisions to accept or deny claims for mental
injury need to be explicit and timely.
Just because a disability insurance policy or workers’
compensation law covers disability due to mental injury does not automatically
mean an immediate and complete filing of such claims. There are many societal
and process factors that may inhibit a worker with a work-related mental injury
from filing one. The stigma associated with mental injury and mental illness
more generally is a big one.
Stigma
The stigma associated with mental injuries may
discourage those in need from seeking treatment or attributing disability to
other causes to avoid real or perceived stigma. While measuring attitude
assesses the societal or workplace environment, stigma is best assessed from
the perspective of individuals experiencing mental illness or injury.
Those seeking help through the healthcare system report
feeling patronized, punished, or
humiliated (Christina Pellegrini, Mental illness stigma in health care settings
a barrier to care, CMAJ January 07, 2014 186 (1) E17).
Public education programs and industry-specific initiatives to de-stigmatize mental injury
will “reveal” underlying cases of work-related mental injury. It may increase
claims for workers' compensation, but that does not automatically lead to increases in
accepted claims.
Successful efforts to reduce stigma will increase
claims statistic for work-related mental injury and disability in two ways. Those
injured or suffering from mental conditions may seek help directly because of
the mental injury and cases previously initiated for other causes may be
recorded as having a primary or secondary mental injury component.
As with attitude, stigma levels vary greatly. Few local
or workplace surveys assess stigma, but elevated levels of stigma are likely to
suppress claims, prolong disability, and worsen outcomes.
Overcoming the stigma issue is just one step. Choosing
to file a workers' compensation claim is
quite another, one that involves processes that may be harmful or so onerous as
to cause a worker to avoid reporting the mental injury altogether.
The following touches on just a few process issues.
Workers' compensation coverage for mental injuries
The mental injury category of work-related injuries is
more complicated than most other injury categories. Keep in mind, each
jurisdiction will have its own characteristics that make direct comparative
analysis difficult.
The inter-jurisdictional differences in reporting
requirements and coverage may influence the willingness of parties to report
mental injuries. Even within jurisdictions, the reporting and coverage of
mental injuries is subject to a lot of change.
The following highlight just a few sources of difference and how these
may impact jurisdictional data over time and complicate interjurisdictional
comparison.
Processes
for filing and adjudicating claims
All workers'
compensation claims are evaluated based on the connection between injury or
illness and work. Legislation in each jurisdiction is specific to that
jurisdiction and may include provisions such as exclusions and presumptions
regarding mental injuries but operational processes can also have a big
impact.
Adjudicative practices directives, staffing levels and
organizational factors can all influence how claims are processed and
adjudicated. Some jurisdictions take a generalized approach while others have
specialized adjudicative and administrative sections to manage mental injury
claims. The specialized structures tend
to have specific training and procedures that may be more accommodating to
those with mental injuries.
The adjudicative framework will also impact both the
acceptance rate and the willingness to file a workers'
compensation claim for a mental injury. That framework often depends on
external definitions as well as internal applications (policy, practice,
administration).
Changing
definitions and the PTSD example
Definitions in legislation and associated with coding
systems change over time. One example is International Classification of Disease (ICD)
system is commonly used to code claims. ICD-9 had 14,000 codes and was used for
decades; its successor, ICD-10, has 70,000 codes and has been used broadly
since around 2015. Other coding systems for nature of injury, industry and
occupation are jurisdictionally specific and subject to change over time. And
coding practices may or may not be consistent within or between jurisdictions
over time.
Workers’ compensation systems rely on a medical diagnosis of the injury, then determine the "work-relatedness" of that injury before considering the extent and
duration of any compensation. Changing definitions can play a role in the
process and what is reflected in statistical data. Here is one example.
Post-Traumatic
Stress Disorder (PTSD) is a recent term, but
the condition this term describes has been around for centuries. While "shell
shock", "battle
fatigue", traumatic neurosis or
hysteria were used in the military context in
the 19th and first half of the 20th century, when the
DSM was first published in 1952, it did not contain references to these terms
or PTSD; that changed in 1980.
The original DSM-III (1980) description focused on
external traumatic events, emphasized etiology, and had narrow exposure
criteria. The DSM-5 (2013) changes broadened the exposure criteria and expanded
symptom clusters. The changes reflect a growing understanding of PTSD.
I started working in vocational rehabilitation in the workers' compensation context in 1980. It was clear to psychologists
I worked with that some of the workers we encountered were suffering from PTSD.
I also recall that acceptance of claims for PTSD took effort and depended, in large part, on
just getting the worker assessed by a qualified professional. Few cases were considered,
fewer were accepted.
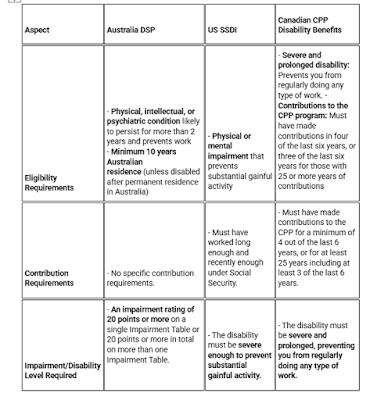
To be clear, certain
psychological disorders as sequelae to physical injury are accepted by workers' compensation systems in the US, Australia, and Canada
because of a clear nexus between the direct physical traumatic and the mental
injury. The recognition of a disabling condition in the absence of physical
trauma is more recent.
The point here is that changing definitions may account
for more cases considered and recorded as mental injuries. More practitioners
recognize the harm, more legislation addresses the issue, more administrative systems record the data in the mental injury category either
as a primary, secondary, or other diagnosis.
How common is PTSD?
Increases in mental injury statistics are not necessarily reflective of a worsening work environment. Definitions and criteria for PTSD have changed over time. Reduced stigma and increased awareness contribute to more cases being considered and identified. Better legislation, policy and practices will also contribute to the increase. That begs the question, will the level of PTSD and other mental injuries level off? If we are recognizing, adjudicating, and recording cases optimally, the levels will more closely reflect actual prevalence.
While most people will not develop PTSD as currently
defined, the prevalence may be greater than you might expect. According to the US
National Center for PTSD, about six out of every one hundred people (or 6% of
the U.S. population) will have PTSD at some point in their lives—8% of women
and 4% of men. [see “How Common Is PTSD in Adults?” at https://www.ptsd.va.gov/understand/common/common_adults.asp ].
Of course, these data do not differentiate causes (for
workers’ compensation) or numbers within the working population (for disability
insurance, social insurance plans). With treatment, symptoms typically subside
below the diagnostic threshold.
Exclusions
and Presumptions
Disability insurance policies may exclude certain conditions
or risks. Pre-existing conditions may preclude coverage of disabilities related
to mental illness or disorder. Workers’ compensation systems may also have
specific exclusions and presumptions.
Workers’ compensation legislation sets the parameters
for the acceptance of mental injuries. Many laws have specific exclusions that
further hinder direct inter-jurisdictional comparisons. For example, the Workers
Compensation Act in British Columbia has an "employment
exclusion" (section 135(1)(c)) that accepts mental disorders as compensable only if: "the mental disorder is not caused by a decision of the
worker's employer relating to the worker's employment, including a decision to
change the work to be performed or the working conditions, to discipline the
worker or to terminate the worker's employment." While
variations of the employment exclusion are common, other statutes include "presumptive"
clauses that may be applied very narrowly or quite broadly. In 2018, Nova
Scotia included a presumption for frontline and emergency response workers
diagnosed with PTSD. The presumptive cause makes it easier for these workers
because the condition is presumed to be work-related. [see PTSD Presumption for
Frontline or Emergency Response Workers - Government of Nova Scotia, Canada]
Queensland's Workers'
Compensation and Rehabilitation Act 2003 now includes Subdivision
3BA PTSD sustained by first responders and other particular persons and extends
presumptive work causation to those whose "employment
requires the person to experience repeated or extreme exposure to the graphic
details of traumatic incidents by— (i) attending the scenes of traumatic
incidents; (ii) experiencing traumatic incidents as they happen to other
persons; (iii) investigating, reviewing or assessing traumatic incidents that
have happened to other persons."
Presumptive clauses remove the need for the worker to prove work-relatedness or
the decision-maker to make complex and difficult inquiries into individual
cases to determine causation. Most presumptive clauses are rebuttable if there
is sufficient weight of evidence to the contrary.
Presumptions may increase claims filing, and exclusions may increase denial rates and suppress filing claims. These factors will vary by jurisdiction
and within jurisdictions over time, making
comparisons between jurisdictions or over time within a jurisdiction more
difficult. The exact provisions for presumptions and exclusions can only be
determined by workers’ compensation authorities. It is no surprise that disability
insurers often require their claimants to file workers’ compensation claims.
Varying
onus and standards of proof
The onus of proof refers to the responsibility of presenting evidence to support a claim. Who bears that onus varies, and that can impact claim-filing behavior. It is common to encounter injured workers for whom the perceived obstacles to filing a claim result in their declining to even report serious physical or mental injury.
Inquiry-based jurisdictions, such as those in Canada
and some US states, often place the onus on the adjudicator or the workers'
compensation board. This approach recognizes the inherent imbalance of power
between the claimant and the employer or insurer, and it aims to ensure a fair
and comprehensive investigation of the claim. For instance, in Ontario, Canada,
the Workplace Safety and Insurance Board (WSIB) has a statutory obligation to
investigate and make decisions based on the merits and natural justice. The
adjudicator is responsible for gathering relevant evidence, seeking expert
opinions, and deciding based on the evidence presented.
In contrast, in more adversarial jurisdictions, the
onus rests on the claimant. This is the case in many jurisdictions in the
United States, where the claimant must provide substantial evidence to support
their claim for mental injury. For example, in California, the claimant must
prove that the mental injury was predominantly caused by actual events of
employment, rather than by non-industrial factors.
The variability in reported incidence of mental
disorders in workers' compensation may be due in
part to variations in the standards of proof. The standard of proof refers to
the level of certainty required to establish a particular fact or claim.
Different jurisdictions may employ different standards of proof for mental injury
claims.
The "causative significance" standard is used
in some Canadian jurisdictions. Under this standard, if the work-related
factors were a significant cause of the mental injury, even if other
non-work-related factors also contributed, the claim is accepted.
The "balance of probabilities" standard is
commonly used in many jurisdictions, including some states in the United States
and some provinces in Canada. By this standard, the claim is accepted if it is
more likely than not that work-related factors caused the mental disability.
The "predominant cause" standard is more
stringent (for example, New South Wales,
Australia). Under this standard, the
claim is accepted if work-related factors are the primary or predominant cause
of the mental injury, outweighing all other non-work-related factors combined.
More stringent onus and standards of
proof factors may discourage claims rather than increase denial rates, which
are rarely published by injury category. In any comparative analysis,
understanding these factors is critical.
Limitations
on Compensation and Disability Insurance
Mental injuries may take a long time to develop,
diagnose, adjudicate, treat, and compensate. That passage of time, the
complications of filing, effort in seeking claim acceptance on top of
recovering from the mental disorder make it challenging. More than one worker has said, “Claiming
is not worth the pain.” This “hassle”
factor is an inherent limitation in the process and leads to fewer claims being
filed and more being abandoned.
As for the issue of permanent disability compensation
for mental injuries, the application of proportional causation, particularly as
used in California, is noteworthy. In California, if a mental injury is found
to be compensable, but it is determined that both work-related and
non-work-related factors contributed to the injury, the disability compensation
may be proportionally allocated based on the degree of each factor's
contribution. On one hand, this approach acknowledges the complex nature of
mental injuries and ensures that claimants receive appropriate compensation
based on the factors involved in causing their condition. On the other hand, apportioning
causation is difficult, arbitrary, and counter to the no-fault principle fundamental
to workers’ compensation.
Again, the process of obtaining the information needed
to determine causation is intrusive and may discourage initial applications or
increase abandonment of efforts to complete a claim.
In both the workers’ compensation and disability
insurance domains, limitations may include certain age and duration
restrictions for some or all benefits including those involving mental injury
or disability. Common LTD benefits for mental illness last only 12 to 24 months.
Integration with social insurance plans or other coordination of benefits may
limit compensation and benefits. These limitations vary by jurisdiction and may
alter the incentives and disincentives for claim filing.
Understanding the limitations and any change in
legislation or policy that limits access or the amount of compensation is
important to understanding the apparent mental injury claim rate.
Societal
and Environmental Factors Play a Role
As noted in the attitudes and stigma sections, the
societal environment is critical to understanding trends in work-related mental
injury data. Here are a few other factors to consider.
Diagnosis and treatment of mental disorders are complex
and complicated by the barriers that may exist in accessing mental health care
professionals. Many jurisdictions have a shortage of qualified psychologists
and psychiatrists—professionals often required to make the diagnosis that
initiates a claim. Some jurisdictions are broadening the scope of practice of
related professions to broaden access to treatment, typically under the
direction of a supervising senior professional.
If the societal or operational expectation is for a
manager to be available 24/7 or a factory worker to work 9-9-6 (nine AM to nine
PM six days per week)—even if that is counter to official labor laws—workers
may feel compelled to comply just to retain employment or secure advancement.
Certain professions have a culture of just forging ahead despite knowing the
health risks. These factors can impact the apparent data on mental injury
claims and contribute to increased incidence of mental injury.
As with culture, attitudes, and stigma, other societal
factors inherently influence the mental injury data. Although inter-jurisdictional comparisons can adjust for industrial
mix and demographic factors, contextual social factors cannot be ignored.
What
about Prevention?
While the focus of the statistics in this discussion is
on injuries, fatalities through suicide are a terrible but real consequence of
mental injuries. Primary and secondary prevention must be considered.
There are some obvious primary prevention initiatives
that can reduce the incidence of work-related mental injuries. We may not be
able to eliminate the inherent pressures in the unpredictable events in a
first-responder's job, but controlling
exposures to predictable stressors such as overwork is possible.
Building resilience and reducing the stigma associated
with mental injuries takes some effort. BC First Responders' Mental Health
conferences and workshops and Australia's Mates
in Construction are examples of such efforts.
As noted, access to diagnosis and treatment is
challenging. Certain interventions such as cognitive-behavioral therapy (CBT)
have good evidence of effectiveness but are costly with limited professionals
providing treatment. Expanding and expediting access to these resources may
well reduce the number of disabling mental injuries and the duration of claims.
Supports in the workplace for return-to-work are critical to this and may
prevent worsening symptoms and outcomes. Effective vocational rehabilitation is
also important where occupational change is necessary to achieving a safe,
durable return to work.
Where
Will the Trend Go from Here?
The research evidence has firmly established the work-relatedness
of many mental injuries. More research is needed,
particularly around risk factors, early interventions, and treatments. That
research may impact the human and financial costs of work-related mental
injuries.
Workers’ compensation jurisdictions are more accepting now
of claims of mental injuries than twenty years ago. Workers' compensation jurisdictions and their appellate levels
will continue to develop their laws, policies, and jurisprudence to recognize
mental injuries. Those trends will also have consequences.
Recognition will logically lead to increased claims.
Raising awareness will lead more individuals and their health-care
professionals to make the link between work, injury, and disability.
Destigmatization of mental injuries more generally in society will also
contribute to increased workers' compensation claims. The
scarcity of treatment options and the cost of treatments could contribute to
increased claims; however, many workers have told me that the added stress of
pursuing a workers' compensation claim is a
huge disincentive to establishing a mental injury claim.
Despite the inherent barriers and “hassle factor” in
filing a workers’ compensation claim, the growing recognition of the work-relatedness
of many mental injuries may continue to drive disability insurers require filing
of workers’ compensation claims as a condition of STD or LTD coverage wherever work
be a factor.
For jurisdictions well along in the acceptance of
work-related mental injuries, the trend
lines may level off or decline. Mental injury from overwork, bullying, and harassment are amenable to prevention
strategies, although awareness building may increase claims initially.
For jurisdictions early in this evolution, you are
likely to see rising claims for a time before the proportion of work-related
mental injuries stabilizes.
All jurisdictions should consider increased research
investments. As with other work hazards, we know primary and secondary
prevention can be effective, but
knowing which interventions have the greatest benefit takes effort.
Operationally, improved access to diagnostics and treatment is critical, particularly in reducing the severity and duration of
disability arising from mental injury. Achieving that may involve greater inter-jurisdictional cooperation and investment in
programs to develop and train more professionals and technologies.
The reality of work-related mental injury has never
changed. Recognition of that reality is changing. Hopefully, the prevention,
diagnosis, treatment, and rehabilitation can improve to address the real needs
of the people and communities beyond the trend lines.