skip to main |
skip to sidebar
I was asked a few weeks ago how I would design a workers’ compensation system. I’ve actually given this a lot of thought over the years and have come up with some principles that I believe would optimize a new workers’ compensation system in a society similar to the Canadian context. Before you even glance at the following statements, let me make one point crystal clear. I am not advocating any existing system change to adopt any of the following items. This is just a conversation starter intended to help in a ‘green field’ exercise. Each item in the list is in some way dependent on others so the list is intended to be applied in its entirety to a hypothetical jurisdiction. Remember, these are my personal opinions based on my own experiences and observations; these items are not intended to be a statement of direction for WorkSafeBC or a prescription for any other existing system. Let me also add that each item here could fill pages of discussion and analysis. I would be happy to discuss any one of them. Finally, the list is not comprehensive. There are lots of other items that I would add for the design of a complete system but that is beyond the scope of a personal blog.Keeping that in mind, here are my top dozen design criteria/features for such a hypothetical new workers’ compensation system in a society similar to Canada:1. Prevention orientation: This has to be at the top of the list. Employers would be required to report all work-related injuries to the agency within three working days.
2. Universality: Every worker and employer should be within the scope of coverage… and all work-related injuries, illnesses and diseases should be included within scope. This takes away workers’ rights to sue but creates a comprehensive no-fault coverage system.
3. Integrated: Given the universality of coverage, it makes sense to combine and integrate the compensation and prevention (consultation, education, promotion and compliance enforcement) functions. It also makes sense to have the rate-making and financial authority integrated into this model.
4. Accessibility: workers and employers should have instant electronic access to information about their claim or claims, be able to communicate, and transact all business with the workers’ compensation insurer without temporal, language, bureaucratic or other barriers.
5. Actuarially based: full funding (capitalization of costs) for injuries should be maintained by injury year (premiums should cover all incurred costs including prevention and future administration).
6. Comprehensive: All medical diagnostic, treatment, and rehabilitation (physical, social, psychological and vocational) should be covered. This ensures that the costs of injuries are born by industry and not the taxpayer. It also is consistent with the current Canada Health Act, which does not include payments made by a workers’ compensation system in the definition of an insured health service.
7. Supporting of the worker-employer relationship: all claims of less than 8 weeks should be paid directly to the worker by the employer (at the prescribed rate). The employer would be reimbursed by the workers’ compensation agency dollar-for-dollar for all wage-loss benefits paid to the worker through week six of the claim.
8. Supportive of complete claims reporting: Experience rating would not apply to claims of less than 8 weeks duration; this creates an incentive for firms to report all injuries (employers get to recover what they spend on wage-loss benefits they paid the worker) while retaining the experience rating that most employers feel adds a fairness to the system for those with poor performance.
9. Encouraging of early and safe Return-to-Work: Employers will be directly responsible for wage-loss costs payable in week 7 and 8 of every claim. Experience Rating will apply for claims of greater than 8 weeks duration. These features provide incentives for early return to work and accommodations consistent with Disability Management procedures.
10. Value the injury of all workers equally: Experience rating based on duration of disability not cost. This avoids the criticism that most experience rating systems are cost-driven and thereby devalue injuries to low wage earners.
11. Compensate long term claims equitably: Permanent Disability (not impairment) to be roughly comparable for workers with similar age, gender, education, industry, and occupational backgrounds relative to their counterparts without work-related injury.
12. Credibility and independence in all classifications: Pools of firms with similar risks should be self sustaining for the costs they incur. Very limited possibilities for cross subsidization and re-insurance.
I repeat, these features are the general parameters and very brief rationales for a new system and are not intended to be a roadmap for reform of any particular system. Any system is a product of its history, societal values, politics, and even geography. The present design of any system is responsive to a particular environment. I am not injecting these ideas into any particular reform process.
I have conveniently left off how dispute resolution mechanisms would operate, how premium rates would be established and what one would do with exceptional cases (this is only a blog post, not a thesis).
Perhaps you have your own ideas. I would be interested in how you would design a system if you were starting from scratch.
Duration of disability is a complex measure within workers’ compensation systems. Duration has natural drivers such as age (it takes longer to recover as we get older), injury type (more severe injuries take longer to recover), and even obesity (obese of workers as a group take longer to recover than non-obese workers with similar injuries) can drive duration higher. We can’t do much about these drivers once an injury takes place. After an injury, there are some things we can do to speed recovery and militate against excessive duration. We have strong disability management programs that can speed return-to-work (assuming the programs are well staffed, the staff well trained in DM principles, and stakeholders are willing to support DM efforts). There are guidelines for expected recoveries and programs that encourage early and safe return to work (research literature shows that work is actually good as therapy and contributes rather than works against good health). Medical science and physiotherapy have advanced dramatically over the last century and each of these can contribute to more rapid recover and return-to-work outcomes. External factors put pressure on duration. In a slowing economy, durations tend to rise. This makes sense since workers not on wage-loss benefits are likely in a position to carry some of the extra load at no direct or current cost to the payroll. Rising and hot economies tend to contribute to shorter duration. Workers are enticed to return to work and are more likely to be accommodated by their employers in these circumstances. Access to healthcare can also delay recovery. If it takes a year to get an MRI and six months to see a surgeon, you can bet that duration statistics will rise. Despite these factors, it appears some general measures of duration of disability from work-related injury have remained remarkably stable over time. In Sir William Meredith’s Final Report, Meredith muses “…it may, I think, fairly be assumed that the great bulk of the accidents for which compensation would be payable under the proposed law will incapacitate the workman for short periods—84 per cent probably for less than fourteen weeks.”I looked at WorkSafeBC claims with an injury date in 2008 where there was at least one day away from work. WorkSafeBC pays wage-loss benefits beginning the day following the day of injury so our way of counting may not fully match with Meredith’s assumption. That said, his projection looks pretty good— 85.14% of time-loss claims with an injury date in 2008 had durations of less than 14 weeks. One factor contributing to the relative stability of duration is the common denominator of human biology and physiology. Healing times have not really changed over the last 100 years for many conditions. Fractures still take the same time to mend; lacerations take about the same to heal. Yes, we have antibiotics and new technology. These save lives. Many victims of severe injury would not have survived in Meredith’s time. They survive today… but their recovery and return to work can take a lot longer. I’ve also looked at duration by age category. Over the last couple of decades for which I have data, the average duration for 20-24 year olds or 35-40 year olds has barely changed. What has changed is the demographic mix with older workers now dominating the distribution of injured workers. This change in mix is another factor that will continue for some time to put upward pressure on duration. Of all the factors listed, effective disability management is the leading candidate to counter the upward pressures on duration.
Premium or Assessment Rates in workers’ compensation are a unique comparator. Because they are normally presented in North America and Australia as $x.xx per $100 of (assessable) payroll, it is trivial to convert this to a standard percentage (x.xx%). A percentage is independent of currency so it is possible to compare jurisdictions in different countries without worrying about exchange rates. Time series of assessment rates may also tell a story. Since rates are ultimately based on incurred costs, rising rates usually indicate rising costs within the sector covered by the premium or assessment. This holds true for most systems. For example, rates may rise if experience shows that injuries are resulting in increases in severity. Other explanations are also possible.I recently resurrected some notes I had copied from Sir William R. Meredith’s Interim Report on Laws Relating to the Liability of Employers (1912). In that report is a table of Premium rates for employers in their industry ‘mutual funds’. As you may recall, the German system at the time consisted of employer mutual insurance funds for workers’ compensation organized by sector. Bismarck proposed the system in the early 1880s and the time series in Meredith’s interim report covers the period 1886 to 1908. Many of the rates changed over the time series. This is understandable because the first year would have been an estimate. Over time, as experience was gained, more accurate estimates of cost could be made. This would lead to more accurate premium rates. Meredith notes that the German rates include a nine to ten percent margin above the cost rate to establish reserves funds to cover unforeseen contingencies such as “the entire wiping out of the industry or its inability to meet its payments in a period of financial depression”. There is a lesson there for many systems.How much have things changed since then? The following chart lists the Assessment Rates for Germany for selected sectors in 1886 and 1908 (bars) with the current (2010) WorkSafeBC premium rates (points connected with a line).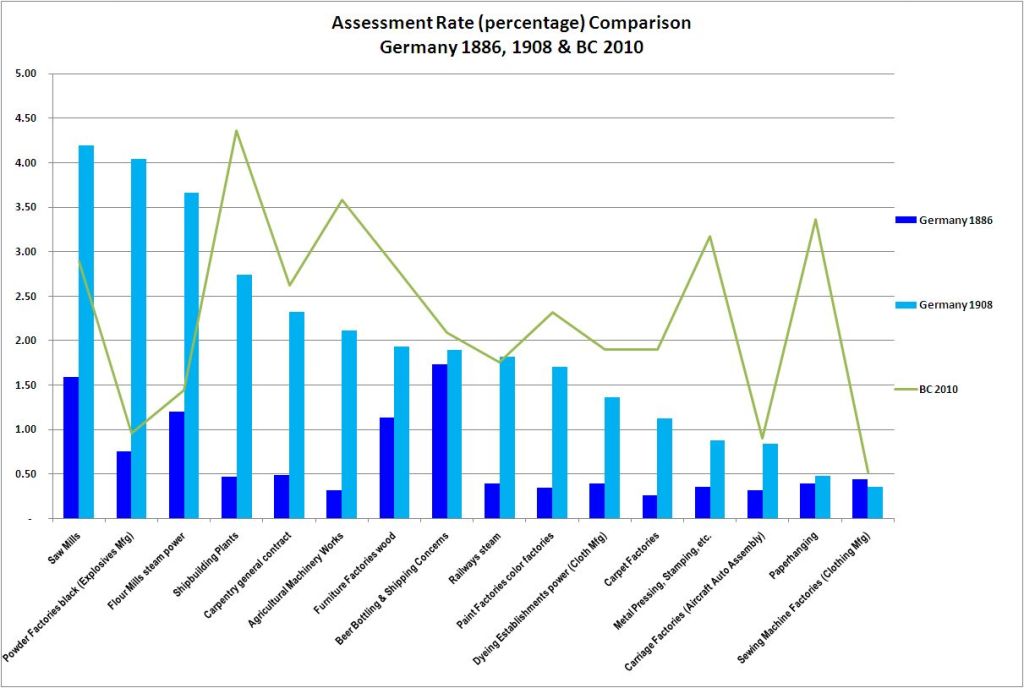 Looking only at the German rates, one can see that most rates rose over the first two decades. By comparison, using our modern classifications with some adaptations (like substituting ‘Aircraft Automobile Assembly’ for ‘Carriage factories’), about half the rates are near or below their German counterparts’ 1908 levels. This is understandable with respect to some sectors such as sawmills where technology has made amazing progress in terms of safety and health. Other sectors have increased in costs. The explanations here might relate more to increases in scope of coverage (to include occupational diseases such as asbestos-related conditions in shipbuilding). Comparing systems is always problematic and comparing different systems more than a hundred years apart is an admittedly dubious enterprise. It is natural, however, to ask how the rates of one system compare to another particularly at the industry level even if widely separated by time; most of us need that perspective as a starting point. What surprised me was that premiums today are not drastically different than they were a century ago. I don’t believe that the cost of workplace injuries should be considered merely a cost of production. That said, what is striking about the chart is how similar the range of rates appear.
Looking only at the German rates, one can see that most rates rose over the first two decades. By comparison, using our modern classifications with some adaptations (like substituting ‘Aircraft Automobile Assembly’ for ‘Carriage factories’), about half the rates are near or below their German counterparts’ 1908 levels. This is understandable with respect to some sectors such as sawmills where technology has made amazing progress in terms of safety and health. Other sectors have increased in costs. The explanations here might relate more to increases in scope of coverage (to include occupational diseases such as asbestos-related conditions in shipbuilding). Comparing systems is always problematic and comparing different systems more than a hundred years apart is an admittedly dubious enterprise. It is natural, however, to ask how the rates of one system compare to another particularly at the industry level even if widely separated by time; most of us need that perspective as a starting point. What surprised me was that premiums today are not drastically different than they were a century ago. I don’t believe that the cost of workplace injuries should be considered merely a cost of production. That said, what is striking about the chart is how similar the range of rates appear.
A few weeks ago, I attended the International Forum on Disability Management (IFDM) and annual convention of the International Association of Industrial Accident Boards and Commissions (IAIABC) in Los Angeles. This was a great opportunity to hear from other systems about the hot issues, successes and challenges facing systems in the US and other jurisdictions. The following is sampling of what I heard:
- Dame Carol Black spoke about her review and report of the UK system for compensating for work injuries. She has been instrumental in changing the focus in that country to conform to the principles of Disability Management. It was fascinating to hear how engrained the system of ‘sicknotes’ was in legislation and practice. As simple and fundamental as it may seem to us, the move away from this terminology to ‘fit notes’ and a focus on ability has been a big challenge for the country and the transition is still underway.
- The German Social Accident Insurance system (DGUV) is celebrating its 125th year as a Bismarckian workers’ compensation system. It has also undergone a major consolidation from more than twenty industry-specific mutual systems to nine. They are also facing the same sorts of issues we are seeing in North America including a rising tide of occupational diseases and an increase in psychological injury cases.
- In New Zealand, the Accident Compensation Corporation (ACC) is a relatively young system of just 34 years. It covers work and non-work injuries that involve lost earnings. Interestingly, the change in accounting standards (known as IFRS) is creating a new challenge for the system that is driving a lot more attention on long-term claims. The new accounting standard requires the government to carry the expected lifetime cost of claims as a liability.
- Munich Re, the largest reinsurer highlighted its major concerns for the future. Its criteria acknowledge risks like nanoparticles and nanotechnology but did not list them because they cannot yet quantify a cost impact. Of the items that they can make some estimates on, obesity, the aging labour force, the use of temporary foreign workers, psychological injuries, and long latency occupational diseases topped the list.
- On the IAIABC side of the agenda, a presentation from the National Council on Compensation Insurance (NCCI) highlighted obesity. Their economist concluded that there were marked differences in outcomes for obese and non-obese workers who sustain similar work-related injuries. Their analysis of members’ workers’ compensation claims found that injuries sustained by obese workers are more likely to result in permanent disabilities and the range of medical treatments and costs are greater for obese claimants.
- Tungsten Inert Gas (TIG) welding was highlighted by the IAIABC as an emerging issue with respect to its apparent linkage to Parkinson’s disease. There was speculation that this sort of occupationally-specific exposure-linked health condition may well work its way into presumptive clauses in the near future, in part because of pressure elsewhere on medical costs.
- Medical costs came up again in a discussion of the required switch in the US from the medical coding system known as ICD-9 to ICD-10. The change is mandated now for October 1, 2013 having been pushed back several times. The reporting has implications for workers’ compensation systems. There is no general equivalent matching that can be applied to ‘crosswalk’ old codes to new ones. The example used suggested that the code for the amputation of a finger go from one code to more than twenty.
- Finally, we got a preview of data to be released in the Oregon Department of Consumer and Business Services' Workers’ Compensation Rate Ranking Survey. This survey is completed every couple of years. It lists a series of classifications that are the most costly from a workers’ compensation perspective in Oregon. It then applies the rates from other states to that set of classifications and payrolls from Oregon. The result is what the average rate would be in Oregon if Oregon had the other states’ rates. The study should be released in the coming weeks and will likely receive some media attention.
That’s a small portion of what was covered. In the coming weeks, I will have more details on some of these issues.

